Introduction
Klumpke’s paralysis, a condition affecting the lower brachial plexus, often arises from challenging childbirth experiences. This article seeks to provide an empathetic perspective on this neurological condition and the importance of compassionate care.
Unveiling Klumpke’s Paralysis
Klumpke’s paralysis involves injury to the eighth cervical and first thoracic nerves, either before or after they unite to form the lower brachial plexus. This injury can result from stretching (neuropraxia), tearing (avulsion when the tear is at the spine, and rupture when it’s not), or scarring (neuroma) of the brachial plexus nerves. Fortunately, most infants with Klumpke paralysis experience the milder form of injury (neuropraxia) and often recover within six months.
Understanding the Mechanism
The mechanism behind Klumpke’s paralysis typically involves hyper-abduction traction, leading to various signs and symptoms indicative of neurological trauma.
Recognizing the Signs and Symptoms
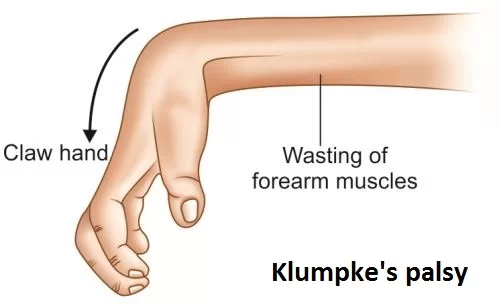
Klumpke’s palsy is marked by:
- Atrophy in forearm or hand muscles.
- The challenging symptom of “claw hand,” where the forearm remains flat, but the wrist and fingers contract.
- Horner’s syndrome, characterized by drooping eyelids on one side of the face.
- Inability to utilize the muscles in the affected arm and/or hand.
- A limp or paralyzed arm.
- Numbness in the affected arm and/or hand.
- Occasional severe pain.
- Stiff joints in the wrist and hand.
- Weakness in the affected arm and/or hand.
Exploring the Causes
Klumpke’s palsy can occur due to difficult childbirth, primarily during vaginal deliveries, especially if the mother is petite, and the baby has a larger birth weight. Gestational diabetes and improperly managed maternal diabetes can also contribute to the condition. Trauma to the arm or shoulder during a fall and tumors in the upper lung and collarbone area are additional causes.
Risk Factors
Several factors can increase the risk of Klumpke’s palsy, including breech births, gestational diabetes, improper delivery methods, large infants born to small mothers, prolonged second-stage labor, injury, and a history of or risk factors for cancer.
Differential Diagnosis
Distinguishing Klumpke’s palsy from other conditions is essential. This includes Erb’s palsy, distal nerve entrapment, thoracic outlet syndrome, apical lung tumors, neurofibromas, disc herniation, shoulder impingement, and fractures.
Prevention
Minimizing the risk of Klumpke’s palsy can be achieved through advanced planning by healthcare providers, ensuring qualified personnel are present during delivery, and employing proper birthing techniques. Effective maternal healthcare during pregnancy, including diabetes management, also plays a crucial role in prevention.
Prognosis
In most cases, infants recover from Klumpke’s palsy within six months. However, more severe cases with nerve tearing can result in long-lasting symptoms or lifelong disabilities.
Treatment and Compassionate Care
Treatment options encompass both non-surgical and surgical approaches:
Non-Surgical Treatments:
- Physical therapy helps in mild cases, improving flexibility, range of motion, strength, and dexterity.
- Medications may be prescribed to alleviate pain and discomfort.
Surgical Procedures:
- Surgery may be recommended if physical therapy yields unsatisfactory results.
- Surgical interventions include muscle transfer, nerve grafts, and nerve transfers.
Recovery
Recovery is a gradual process due to the slow regeneration of nerves. Home-based rehabilitation exercises play a vital role in enhancing strength and range of motion post-surgery.
Conclusion
In the journey of Klumpke’s paralysis, compassionate care and a supportive approach are paramount. We stand with those facing this challenge, offering guidance and hope for a brighter tomorrow.
At Ephysioneeds Academy, we offer comprehensive training for physiotherapists looking to progress their skills. Our courses include dry needling certification, advanced physiotherapy techniques, and sports injury treatment. Our rehabilitation certification and physiotherapy training online provide flexibility and depth. We moreover specialize in manual therapy courses and soft tissue therapy certification. Explore our sports fellowship in physiotherapy and detailed A-Z knee and shoulder treatment courses. Additionally, the Tapedia Taping Encyclopedia is an essential resource for mastering taping techniques.